Table Of Contents
Introduction
The Hib vaccine stands as one of the most significant advancements in modern medicine. This vaccine targets infections caused by Haemophilus influenzae type b, a bacterial organism known to cause severe meningitis and other serious illnesses in young children. By offering robust protection from an early age, the Hib vaccine has transformed the public health landscape, drastically reducing the incidence of bacterial meningitis and throat infections in vulnerable populations. In this article, we will explore the details of the Hib vaccine including its vaccine type, the recommended infant series, dose timing, and the importance of booster shots. Our goal is to provide comprehensive insights for both parents and healthcare professionals seeking effective prevention methods against these serious illnesses.
Understanding the Hib Vaccine
The Hib vaccine is specifically designed to combat Haemophilus influenzae type b, a bacterium that once led to a high rate of serious infections, especially meningitis in young children. Through extensive research, it has been observed that routine immunization in infancy has greatly reduced the burden of diseases associated with this bacteria. Below, we discuss why this vaccine continues to be a cornerstone in pediatric healthcare:
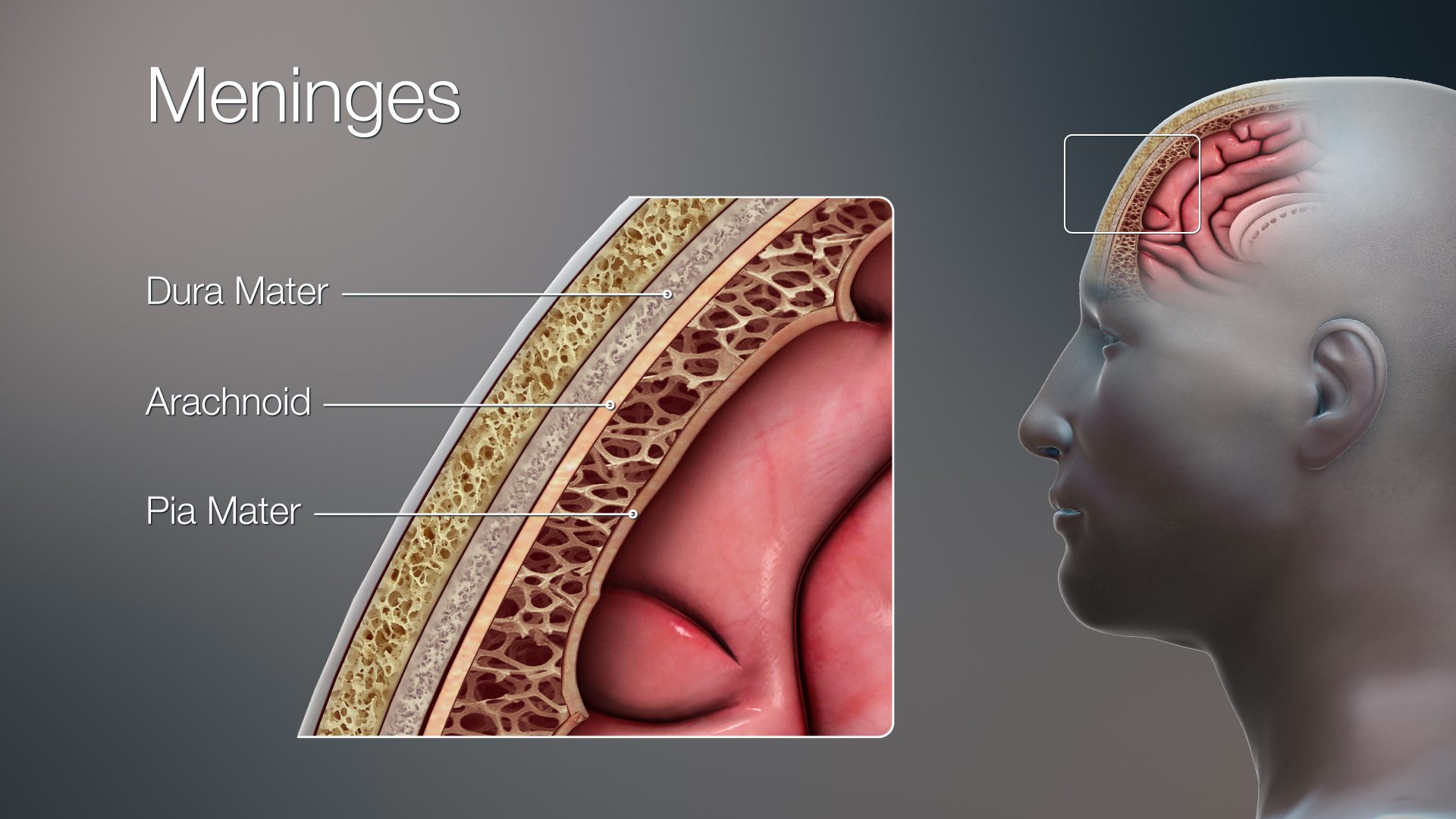
- Prevention of Bacterial Meningitis: The vaccine protects against meningitis, a life-threatening infection of the lining covering the brain and spinal cord.
- Reduction in Throat Infections: Besides meningitis, Haemophilus infections can cause serious throat issues, which the vaccine helps to prevent.
- Overall Child Health: Early vaccination ensures a robust immune system in infants, reducing the chances of serious illness from various strains of bacterial infections.
The Importance of the Infant Series
The success of the Hib vaccine largely depends on the timely administration during an infant’s critical developmental period. The immunization schedule typically involves a series of doses to ensure a strong and lasting immune response. Not only is the initial series crucial, but the timing and combination of doses also play an essential role in creating immunity against the bacterial threat.
Recommended Administration Schedule
Most healthcare guidelines recommend that the vaccine be given in multiple doses starting from 2 months of age as part of the infant series. This early start allows the body to begin building defenses against Haemophilus, significantly reducing the risk of bacterial infections like meningitis. Furthermore, the schedule is specifically designed to accommodate the immune system’s developing nature, ensuring that each dose builds upon the last for optimal protection.
For instance, a typical schedule might include doses at 2, 4, and 6 months of age followed by a booster during the second year of life. This regimen ensures that the child remains protected during the period of greatest vulnerability.
Exploring Dose Timing and Booster Shots
Precise dose timing is critical when administering the Hib vaccine. Adhering to the recommended schedule maximizes its efficacy and ensures that infants and toddlers develop immunity before they are exposed to the bacterium.
How Dose Timing Influences Vaccine Effectiveness
Each vaccine type, including the Hib vaccine, has a specific window in which it should be administered to yield the best immune response. The initial doses provide the primary immune system stimulation, while the booster shot reaffirms and prolongs this immunity. Missing a scheduled vaccine dose can leave a gap in protection, increasing the risk for reaching a threshold level where the bacteria might cause a serious illness.
For example, if a dose is delayed, it may allow the bacteria to begin proliferating, potentially leading to a serious infection like bacterial meningitis. Healthcare professionals stress the importance of following the precise timeline to avoid such complications.
The Role of Booster Shots
After completing the infant series, a booster shot is recommended during the second year. This booster is crucial because it reactivates the immune system’s memory, providing long-term protection against Haemophilus infections. Booster shots help mitigate any decline in immunity and ensure that even as a child’s immune system matures, they remain safeguarded against possible exposure to the bacteria.
Vaccine Type and Its Mechanism of Action
The Hib vaccine is an example of a conjugate vaccine—a type of vaccine that links a weak antigen with a stronger carrier. This process effectively enhances the immune response, especially in young children whose immune systems might not otherwise react as effectively to polysaccharide antigens.
How Conjugate Vaccines Work
In the case of the Hib vaccine, the bacterium’s outer shell, which usually would not invoke a strong immune reaction in infants, is chemically linked to a protein carrier. This conjugation process makes the antigen more recognizable to the immune system, leading to a robust protective response. Consequently, even a small amount of antigen can boost immunity and provide long-term protection against serious bacterial infections.
Actionable Insight: Understanding the science behind the conjugate vaccine can help parents make informed decisions regarding immunization schedules and recognize the importance of booster shots in maintaining immunity during early childhood.
Prevention of Serious Illness Through Vaccination
One of the primary benefits of the Hib vaccine is its role in preventing severe illnesses, particularly those involving the central nervous system. Prior to the widespread use of this vaccine, bacterial meningitis was a leading cause of morbidity and mortality among children. With today’s immunization protocols, the incidence of such conditions has been dramatically reduced.
Impact on Public Health
The introduction of the Hib vaccine has not only decreased the number of cases of bacterial meningitis but has also lessened the overall burden on healthcare systems. This improvement in public health metrics highlights the success of vaccination programs and underscores the importance of maintaining high vaccination coverage within communities.
Regular immunization using the Hib vaccine serves as a shield, protecting children from throat infections, bacterial complications, and other potentially hazardous conditions. Moreover, it contributes to herdimmunity, lowering the risk of disease transmission even among those who cannot be vaccinated.
Case Example
Consider the scenario of a young infant in a community with robust immunization programs. By completing the full infant series of Hib vaccinations according to the prescribed dose timing, the child gains significant protection against serious bacterial diseases. Even if there is a local outbreak of meningitis, the child’s immune system is well-prepared to fend off infection, dramatically lowering the risk of a life-threatening situation.
Actionable Insights and Best Practices for Parents
For parents, keeping abreast of the vaccination schedule and understanding the benefits of the Hib vaccine can be crucial in safeguarding a child’s health. Here are some actionable steps to ensure optimal vaccination coverage:
- Consult With Healthcare Providers: Early discussions with pediatricians can help determine the best timing for the infant series and subsequent booster shots.
- Follow the Recommended Schedule: Adhering closely to the suggested dose timing maximizes the immune response against Haemophilus bacteria.
- Stay Informed on Vaccine Types: Understanding that the Hib vaccine is a conjugate vaccine can help parents appreciate how even low doses build significant immunity.
- Monitor Child Health: Keep a record of vaccine dates and monitor for any side effects, ensuring timely follow-ups if needed.
- Advocate for Immunization: Encourage family members and community peers to adhere to vaccination schedules, contributing to broader public health and reduction of serious illnesses.
By implementing these best practices, parents can take an active role in their child’s health, ensuring that they are well protected against diseases such as bacterial meningitis and throat infections caused by Haemophilus.
Conclusion
In conclusion, the Hib vaccine represents a vital line of defense against severe bacterial infections, particularly meningitis and throat infections. By introducing the vaccine early in an infant’s life and adhering to the recommended vaccination schedule, including both the infant series and necessary booster shots, parents can provide lasting protection against life-threatening illnesses. Understanding the vaccine type and the science behind conjugate vaccines furthers appreciation of how these tiny doses contribute to a larger public health benefit. Ultimately, routine immunization not only shields children from immediate risks but also plays a crucial role in maintaining community-wide immunity, ensuring a healthier future for all.
Making informed decisions based on timely immunizations and proper dose timing can significantly reduce the incidence of serious illness. Whether you are a parent seeking clarity on vaccination schedules or a healthcare professional advocating for public health, the enduring impact of the Hib vaccine on preventing bacterial meningitis and other complications is clear. Let us continue to prioritize prevention and embrace the proven benefits of immunization to safeguard our communities.